I’m old enough to remember paper medical records. Notes from every doctor’s visit I had as a child were collected in a folder with colored tabs, and I brought it along each time I went in for a checkup. Technology began changing the way these records were kept, as hospitals and doctors’ offices stored patient data on proprietary systems. Even then, however, the system was not very efficient. Switching doctors often meant phone calls to previous providers and multiple attempts to migrate your data between incompatible systems.
Why not have one clearinghouse for all your data that is not only easily accessible by your healthcare provider, but by you—the patient who ostensibly owns the data in the first place?
The devil is in the details, as it always is. Any such repository would become a prime target not only for hackers and identity thieves, but insurance companies, advertisers, and anyone else who could use your data to their advantage. Nevertheless, in the early 21st century, the federal government decided to pursue the idea. As part of the American Recovery and Reinvestment Act of 2009, Congress passed the Health Information Technology for Economic and Clinical Health (HITECH) Act, which promoted the adoption of electronic medical records.
The HITECH Act funded state-based health information exchanges intended to connect these systems and facilitate more efficient delivery of information. It was passed just before the Affordable Care Act of 2010 (Obamacare), which established state-based health insurance exchanges.
The Idaho Health Data Exchange (IHDE) was founded in 2008, shortly before these laws were passed. It was structured as a 501(c)(6) organization, a nonprofit entity intended to invest in technology enabling health data exchange for Idahoans. The original board of directors included the CEOs of St. Alphonsus, St. Luke’s, St. Mary’s, and Kootenai Medical Center, as well as representatives from Idaho Power, Regence BlueShield, Blue Cross of Idaho, Sen. Dick Compton, and Richard Armstrong, director of the Idaho Department of Health and Welfare (DHW).
Armstrong was appointed to lead DHW by then-Gov. Jim Risch in 2007 and stepped down in early 2017. During his tenure, he oversaw implementation of major federal healthcare changes in Idaho, including participating in early debates regarding Medicaid expansion.
As far as I can tell, there was no single vote in the Legislature to create IHDE. Rather, it was formed through executive decisions and negotiated rulemaking. DHW routed funds appropriated through the HITECH Act into IHDE, with approval by the Joint Finance-Appropriations Committee (JFAC) and the Legislature over the course of several years.
The end result was that Idaho, like many states, did not establish the exchange as a state agency. Instead, it relied on a nonprofit model contracted through DHW, allowing public funds to flow into a private governance structure designed to coordinate hospitals, providers, and insurers.
According to a report published by the Legislature’s Office of Performance Evaluations (OPE), the state sent $24.4 million directly to IHDE over the course of its contract, while appropriating an additional $64.9 million for healthcare providers to develop their electronic records systems.
Senate Bill 1393, passed during the 2020 legislative session, contained a large portion of that money. Some $16 million in federal dollars was appropriated under a line item called “IHDE Connections – Opioids.” Sen. Jeff Agenbroad of Nampa carried the budget bill out of JFAC to the Senate floor, where Sen. Scott Grow of Eagle (now co-chairman of JFAC) argued against it, to no avail. He expressed concern that the federal grant was too much, too fast, and was also skeptical of the security of the data exchange. Agenbroad was joined by Sens. Abby Lee and Steve Bair, who argued in support, dismissing Grow’s concerns and saying the appropriation was necessary to comply with federal mandates and ensure the security of patient data.
Fred Birnbaum from the Idaho Freedom Foundation was concerned as well:
It appropriates $16 million of federal money to set up the Idaho Health Data Exchange. Even supporters of this exchange concede its myriad startup problems.
However, what is especially bothersome is the line item described as, “IHDE Connections – Opioids.”
Put simply, this project would put every citizen of Idaho’s health care records into one electronic data-base that the Medicaid Division would have access to. All of the private medical records of every Idaho citizen will be visible to certain government employees. The notion that this is necessary to “combat the opioid crisis,” is a shameful rationale for this massive invasion of privacy.
Finally, it must be noted that having everyone’s medical records in one database will make it much easier to transition to a government-run health care system. There is no necessity for this line item to be included in the Medicaid supplemental.
Watch the full debate here:
History appears to have validated Grow’s skepticism. Just two years following that debate, IHDE filed for bankruptcy. The HITECH grant had run out, seemingly validating Grow’s concerns that disruption in federal funding could lead either to collapse or pressure for state taxpayers to assume more of the burden. According to Audrey Dutton at the Idaho Capital Sun, vendors had already sued IHDE over unpaid debts and were preparing to seize the firm’s assets, which could potentially have included sensitive personal data.
The following year, Dutton wrote a comprehensive essay on IHDE’s tribulations that is worth reading. The exchange had emerged from bankruptcy, but found no bailout in the Legislature. Later in 2023, OPE released its report, which did not mince words:
The Idaho Health Data Exchange was intended to ensure that health records are available for Idahoans when needed. Although it has existed since 2008, we found confusion among state officials about the state’s role with the exchange. We found that the state created the exchange as a nonprofit corporation and did not provide the exchange with enough oversight to fulfill its public purpose. Furthermore, the state did not make full use of its system of checks and balances to ensure cost-effective use of public dollars on contracts with the exchange.
This problem became more apparent when a DC-based consulting company took over managing the exchange in 2019. Millions of dollars were spent on noncompetitive contracts without sufficient transparency and accountability. The state received less than what was promised in its most recent contract with the exchange.

Fred Birnbaum analyzed the report for IFF, calling it another scandal for former DHW director Dave Jeppesen, who had recently resigned.
The report meticulously details the deficiencies in the governance structure as IHDE was set up as a non-profit 501(c)6. Meaning that it was structured to get public funding but with limited oversight from Health and Welfare. Perhaps this was intended by the cross-section of “Big Medicine” stakeholders or was just an oversight. In any case, what we do know is that the exchange absorbed $93.3 million of public funds, 98% of which were provided by the federal government. Of the $91.5 million provided by the feds, $64.9 million went to healthcare providers to “encourage them to develop their systems for electronic health records.”
But what the report does not tell us, is which providers got exactly how much money for precisely what services. These providers are not shielded from scrutiny because they were not paid by the exchange but by the Department of Health and Welfare directly.
He concluded with an implied question: Where did all the money go?
The bankruptcy of the IHDE should serve as a wake-up call to Idaho’s Legislature and the people of Idaho about the dangers of so-called public-private partnerships marching into the state’s healthcare system. This initiative was fueled by federal dollars and did not get the scrutiny it deserved. The Legislature, and possibly the Attorney General, need to do further research into exactly where the money went and possibly what relationships exist between various H&W employees, former employees, and recipients of the nearly $100 million investment by taxpayers.
Sasha O’Connell led the audit of IHDE as part of OPE in 2023, and by 2024 had been appointed to the Division of Medicaid within DHW. In June of that year, she presented the report to an interim meeting of JFAC, explaining that OPE concluded IHDE had been founded without enough transparency and oversight. “We found that, over time, the Idaho Health Data Exchange sort of drifted from the department’s oversight,” she added. Sen. Grow, chairing the hearing, suggested it was more accurate to say that oversight had drifted away from doing its job.
O’Connell noted that IT staff from DHW were never able to independently confirm data security within IHDE, but instead accepted what they believed was a third-party attestation. The audit later found it was not a third party after all, but the exchange’s own IT security officer.
O’Connell also noted that there were two financial relationships between DHW and IHDE at the time. Much of the $93.3 million that flowed through DHW involved pass-through federal grants meant to get the exchange and provider partners up and running. However, DHW also paid IHDE $100,000 per year for access to patient data as a client, in the same manner as a hospital or other provider.
Interim DHW director Dean Cameron warned in April 2024 that DHW would cancel its contract unless the exchange provided extensive audits and policy documentation. DHW found IHDE’s response insufficient and cancelled the data access agreement effective June 30, just as Alex Adams took over as permanent director.
According to Transparent Idaho, the final payment from DHW was $25,000, effective August 1, 2024 (which was in Fiscal Year 2025). The Idaho Department of Corrections (IDOC) continues to pay IHDE for services, but much smaller amounts at a time.
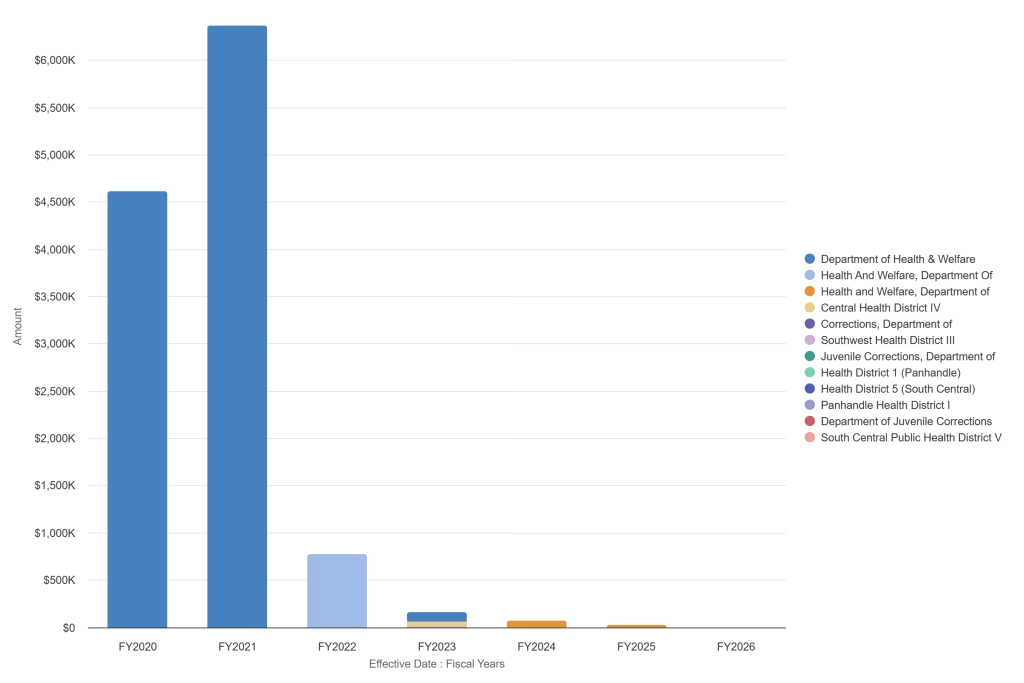
During the June 2024 JFAC hearing, Sen. Grow asked what Idaho had to show for all the money and time invested in the project. O’Connell said the exchange was being used by rural healthcare providers to speed up sharing of patient information, but admitted it never lived up to its full potential.
Rep. Josh Tanner said he had heard from citizens wishing to opt out of the exchange who said they had been unable to do so and had not received responses from IHDE. In his 2024 piece, Birnbaum linked to an opt-out form, but as of this writing the link is broken. IHDE’s FAQ says patients can request to opt out, but includes no specific form.
Now you know the story of IHDE and the greater push for health data exchange up to the present day. Yet many questions remain:
- Where did nearly $100 million in federal dollars go?
- Which providers received money to develop their own databases?
- What is the current status of patient data?
The exchange still exists, relying on subscriber payments from hospitals and other healthcare providers. Former DHW director Richard Armstrong, despite leaving that role in 2017, only stepped down from the IHDE board last December. The current board is a mix of healthcare administrators and other professionals.
While IHDE began as a 501(c)(6), the latest IRS filings appear to show that it is now a 501(c)(3). The 2024 IRS Form 990 shows just $354,000 in assets against more than $2.5 million in liabilities. Executive Director Jesse Meldru received a salary that year of $155,625, while Director of Client Operations Prudence Vincent received $148,125.
The broader question concerns the idea of a health data exchange itself. Is it wise to have a central clearinghouse so hospitals and providers can easily access a patient’s records? If so, should a private entity hold that responsibility, or should there be stronger government oversight? Does IHDE’s lack of revenues suggest there is no sustainable market for the service, or should it be treated, as Civitas Networks for Health CEO Lisa Bari told Audrey Dutton in 2023, as a public utility?
The Legislature appropriated more than $6 billion to the Department of Health and Welfare for Fiscal Year 2026. That is a great deal of money flowing through our healthcare system. As we saw with the Full Circle Health lawsuit demanding Idaho continue paying for HIV treatments for illegal aliens, many figures and organizations have come to depend on that money, with some becoming quite wealthy from it. Such interests naturally want to keep the gravy train flowing, so it is up to us as engaged citizens to help our lawmakers be good stewards of public funds—and that begins with understanding where the money is already going.
Feature image created with Microsoft Copilot
About Brian Almon
Brian Almon is the Editor of the Gem State Chronicle. He also serves as Chairman of the District 14 Republican Party and is a trustee of the Eagle Public Library Board. He lives with his wife and five children in Eagle.